 For the past four years, patients with hand and wrist pain or dysfunction have been able to find the relief they need at UConn Health – without the inconvenience or risk of complications often associated with sedation and general anesthesia.
For the past four years, patients with hand and wrist pain or dysfunction have been able to find the relief they need at UConn Health – without the inconvenience or risk of complications often associated with sedation and general anesthesia.
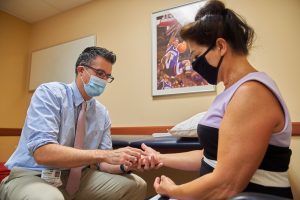
Rather than using a traditional surgical approach, physicians Anthony Parrino, Joel Ferreira, and Craig Rodner – part of the “hand, wrist, and elbow” team at UConn Health’s Department of Orthopedics and Sports Medicine in Farmington – offer “wide-awake surgery” to many of their patients.
This technique, more formally known as WALANT (wide-awake, local anesthesia, no tourniquet), can be used to treat conditions like carpal tunnel syndrome, trigger finger, nerve compression, nail bed injuries, and arthritis. It can also be used to repair ligaments and tendons, repair bone fractures, and remove masses from the hand or wrist.
So how does it work? Prior to incision, the patient’s hand or wrist is numbed up with a small injection of lidocaine – a local anesthetic – and epinephrine, which extends the action of the lidocaine and acts as a vasoconstrictor to control bleeding. No tourniquet or IV is needed. Once the surgery is complete, the incision is bandaged, and the patient’s blood pressure is monitored for a short time before they head home.
Dr. Parrino, who sees patients in both Farmington and Southington, says performing the surgery without sedation or general anesthesia offers a number of important benefits. The first is convenience. Patients aren’t required have a physical beforehand, have preoperative bloodwork done, or temporarily discontinue medications like blood thinners. There’s no need for patients to stop eating or drinking at midnight the evening before their surgery – a huge plus for diabetics, since fasting can interfere with their blood sugar levels.
“I also tell patients that they have the option to drive themselves to and from surgery, if they like, so they don’t have to depend on a ride,” Dr. Parrino says.
 There are other benefits, too. Compared with traditional hand and wrist surgery, patients generally have less bruising and swelling, need fewer pain medications, and find recovery quicker and less painful. And for patients with medical conditions that make them high-risk for anesthesia, WALANT makes it possible for them to have procedures that they wouldn’t otherwise be medically cleared for.
There are other benefits, too. Compared with traditional hand and wrist surgery, patients generally have less bruising and swelling, need fewer pain medications, and find recovery quicker and less painful. And for patients with medical conditions that make them high-risk for anesthesia, WALANT makes it possible for them to have procedures that they wouldn’t otherwise be medically cleared for.
Dr. Parrino says if the procedure involves fracture fixation or tendon repair, having the patient awake allows the surgeon to test the repair during the procedure. “For instance, during trigger finger surgery, I have the patient make a full fist to assess motion. If they have general anesthesia, I am not able to check that active motion and make any needed adjustment.”
The surgery itself is quick; patients are generally in and out of the facility in about an hour and a half. And because they don’t experience the common side effects of general anesthesia – like nausea, vomiting, and fatigue – healthy patients can return to their regular daily activities right after the procedure. Some can even return to work the same or following day, depending on the type of job they have.
Conservative approaches, like braces or injections, are generally tried first, but if those things fail, surgery becomes the next best option.
“And if you come to see us for a carpal tunnel or a trigger finger, 95% of the time, we’re going to recommend a wide-awake procedure for it, as opposed to going with general anesthesia or sedation,” says Dr. Parrino.
An innovative approach
Wide-awake surgery is not common in the Northeast, and while it is available in some metropolitan centers like New York City, surgeons offering it in Connecticut are few and far between.
Dr. Parrino first began practicing the technique during a one-year fellowship at the University of Rochester in upstate New York, after completing medical school at Mount Sinai in Manhattan and his residency at UConn Health. As a resident, he says, “I didn’t really see any surgery where patients are completely awake, and the surgeons are just using local anesthesia.”
 However, on the first day of his fellowship in Rochester, he found himself in the “wide-awake room,” where surgeons were doing 10 to 12 such procedures each day. “I would say half of the procedures I did there were wide-awake,” he says.
However, on the first day of his fellowship in Rochester, he found himself in the “wide-awake room,” where surgeons were doing 10 to 12 such procedures each day. “I would say half of the procedures I did there were wide-awake,” he says.
When he was hired by UConn Health after his fellowship, “one of the things that I wanted to do was to start a wide-awake surgery program. With the help of the orthopedic chairman and some of the staff in the surgery center, we were able to do that, and we’ve continued to build it up.”
His new position gave him the chance to work with Dr. Rodner, as he did during his residency, and with Dr. Ferreira, who got his medical degree at Boston University School of Medicine, and also completed his residency at UConn.
Dr. Ferreira recalls that while he did his hand fellowship at the University of Pittsburgh Medical Center, “I always wanted to come back and teach residents here.” He practiced in Pittsburgh for one year but when a job opened up at UConn, “I took it immediately.”
Today, Dr. Parrino and Dr. Ferreira – an assistant professor of orthopedic surgery – spend a half-day most Fridays conducting wide-awake surgery in Farmington, with each doing approximately 25 of these procedures each month. Dr. Rodner now performs this innovative surgery as well.
Dr. Ferreira says many patients, especially those with underlying conditions like diabetes or cardiac issues, find the opportunity to avoid general anesthesia ideal, “not only for the convenience, but for the safety, too.”
One patient who needed procedures on both hands chose to be asleep for the first surgery, but experienced significant nausea and vomiting afterwards. She chose wide-awake surgery for the second, and it turned out so well that “she was kind of kicking herself that she didn’t do straight local the first time,” Dr. Ferreira says.
WALANT is also less expensive than traditional surgery, since patients don’t require an anesthesiologist.
“It was absolutely amazing”
If you’re wondering what it would be like to be wide awake when your surgeon makes an incision in your hand or wrist and then gets to work correcting whatever has gone wrong inside, just ask patient Janet Smart of Coventry, who underwent not one but three wide-awake surgeries within a short period of time. She can’t say enough about how impressed she was with this new surgical approach. “It was absolutely amazing,” she says.
A few years ago, Smart found that her both hands were painful and numb. She tried hand braces, ice packs and massages, but nothing improved her condition. In early 2019, she finally complained to her primary physician, who told her she was actually losing muscle in her hands and would probably need surgery. Smart then visited Dr. Ferreira at his Storrs office, located about 10 minutes from her home.
After a nerve conduction study showed that she had carpal tunnel syndrome in both hands, Dr. Ferreira offered her the WALANT option. Recalling a bad reaction to anesthesia in her teens, she agreed.
“Dr. Ferreira explained it all to me and drew me a picture of what he was going to do. I love learning about medical things, so it was great being awake during the procedure,” Smart says.
Dr. Ferreira says team members do their best to help put patients at ease. “We have two nurses, Barbra White and Andréa Hunter, who are amazing. And Christine Moran is our wonderful surgical technician,” he adds. “They’re kind of our unsung heroes, because they chat with the patients throughout the whole thing. They’re very calming for anyone who might be feeling nervous.”
Smart was awed by her wide-awake experiences. “The nurses are great. They have music playing in the background, they’re taking your blood pressure, and they’re talking with the doctor. It was just awesome,” she recalls. “Then you get up off the table, you walk down the hall, they monitor your blood pressure for a while, you get your discharge papers, and you drive home.”
She adds, “It was great. No pain. You take a Motrin before you go to bed and the next day, you’re fine.”
Smart’s positive experience is pretty much the norm, according to Dr. Parrino. Although some patients have “looked at me like I was crazy when I first suggested it,” once they learned about the rationale for WALANT and the steps involved, most have been willing to take the leap. “The overall reaction from patients has been very good,” he says, joking, “I have not had anyone run out of the room.”
Prior to surgery, patients are kept in the same general area, separated by curtains. “And even though they can’t see each other, they can hear the people coming back from surgery and realize they’re not in pain – they’re really very comfortable, and they’re talking and laughing. The response from patients after we’re done is, ‘That wasn’t bad at all.’ I haven’t had anyone say they would not do it awake again.”
Because numbing medication is injected only where it’s needed, patients retain full functionality of their hand or wrist, he notes. “They may be a little tingly, but the motion still works,” he says. Once the surgery is complete, the hand or wrist is placed in a padded wrap but it’s not very bulky. “We want them to move their fingers and use their hands for light, normal daily activities. And then on post-op Day 3, we typically will take the wrap off, switch to a Band-Aid, and have them try to get back into their normal routine.”
And what about the recovery period? “Depending on the procedure, there are usually some restrictions for 10 to 14 days until the stitches come out,” Dr. Ferreira says. At the two-week mark, “patients might still be a little sore, but they don’t necessarily have restrictions.”
While some patients may experience some discomfort for up to six weeks, Smart says her first carpal tunnel procedure restored so much function to her hand that she was able to get the other one done within a month. This summer, she returned for a wide-awake trigger finger release.
The surgeries have allowed her to return to her normal activities, after years of dysfunction and pain. “I work part time for the parks and rec department in our town. I clean and mop floors, and I do gardening over there and at home,” she says. “So it’s pretty much back to normal for me, thanks to my dear doctor.”
Carol Latter is Seasons Magazines editor and a freelance writer living in Simsbury.
Photography courtesy of UConn Health
Hear more about wide-awake hand surgery from Drs. Ferreira and Parrino in the UConn Health Pulse podcast






More Stories
Jamie Shawver, D.O.: The Modern-Day Family Doctor
Leading in Urologic Oncology: Ryan Dorin, M.D., Works on Expanding Patient Care
UConn Health Stands at the Forefront of Comprehensive Sickle Cell Treatment in the U.S.