By Steven Blackburn
Dr. Danielle Luciano didn’t just contribute to the successful passage of a one-of-a-kind bill that’s made Connecticut the first state to fully fund endometriosis research for just any reason. She was motivated by her patients. Dr. Luciano and UConn Health, in partnership with The Jackson Laboratory, will soon be operating the first fully state-funded endometriosis biorepository due to that bill.
“After about the 900th time of diagnosing a patient with an incurable disease like endometriosis and being asked, ‘How come this is my first hearing about this?’ or ‘Why didn’t someone else diagnose me with endometriosis sooner?’ you start looking for answers,” said Dr. Luciano, director of the Minimally Invasive Gynecologic Surgery Division at UConn Health.
Endometriosis affects one out of 10 women and occurs when tissue that normally lines the inside of the uterus grows outside of the uterus on various organs. It causes a wide range of symptoms, including infertility and painful menses and intercourse. Very little research has been done on the disease, partly because the U.S. Food and Drug Administration didn’t approve a medication to treat pain associated with endometriosis until 2018. Additionally, few physicians can recognize endometriosis early on or truly understand it. As a result, it can take, on average, seven years for a patient to receive a diagnosis. This lack of knowledge costs the U.S. approximately $20 billion annually to manage the disease, including lost work and school time.
“I originally started researching with Jackson in 2019, and the more we learned, the more complex and poorly researched we realized it was,” said Dr. Luciano. “I really feel like this is an area that needs to be addressed. It affects such a huge percentage of our population that we must research this to better treat our patients.”
Following in the Footsteps of Her Father
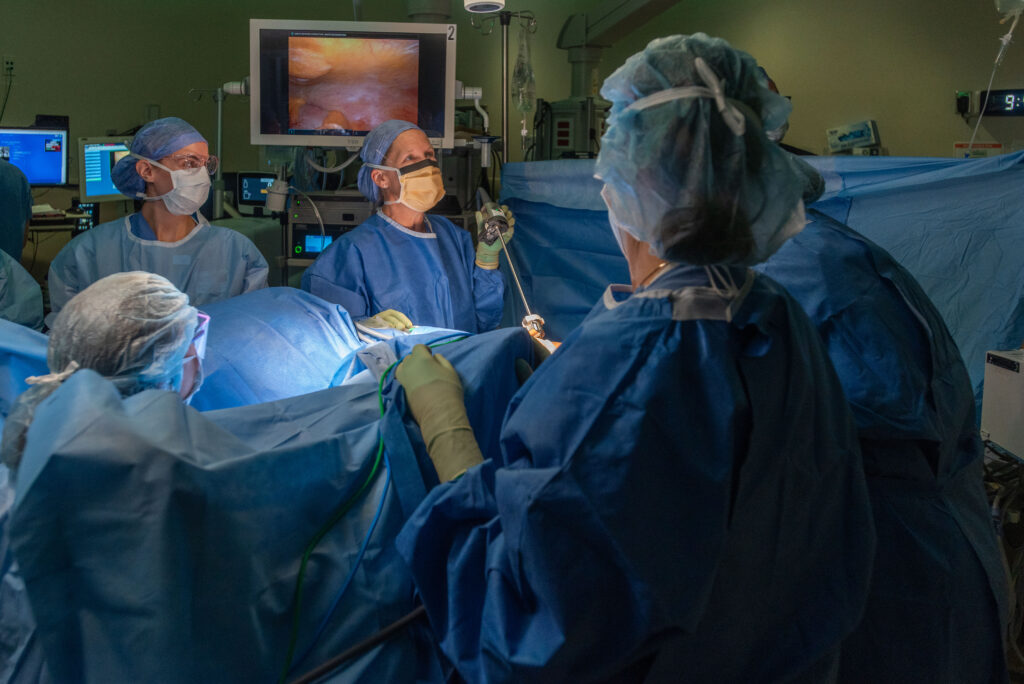
In addition to Dr. Luciano’s patients motivating her to research endometriosis, she entered the fields of minimally invasive surgery, gynecology and endometriosis because of her father. He shared these same specialties until he recently retired. “I wanted to be a doctor like my dad, but originally planned on becoming a pediatrician. Then I fell in love with being in the operating room,” she recalled. “I also really liked women’s health and the aspect of doing surgery but actually getting to stay in my patients’ lives post-surgery rather than never seeing them again.”
During her residency, surgery once again called to her, especially minimally invasive surgery. This choice influenced her later decision to find answers for her future endometriosis patients. “I appreciated performing big surgeries through small incisions so patients could make faster recoveries and return to their regular lives quicker,” she said.
After a two-year fellowship, Dr. Luciano joined her father’s private practice, which eventually became a part of UConn Health in 2014 as an academic center. For the next 4 years, she took more and more responsibilities from her father, who was increasingly eying the alluring prospects of retirement. She eventually assumed the director’s role she has now, which involves treating endometriosis.
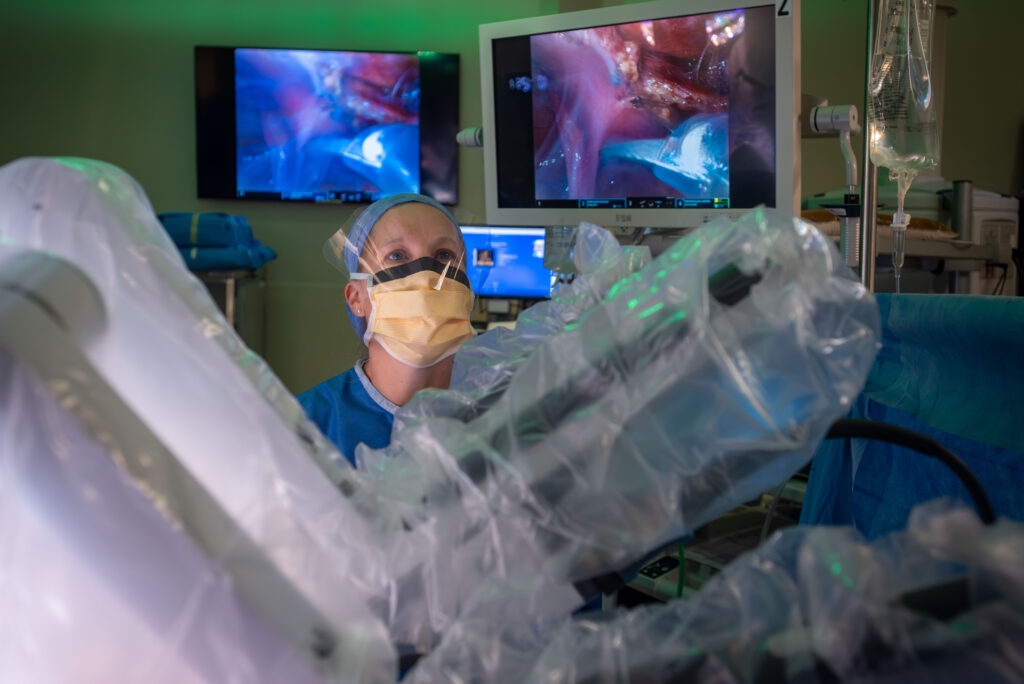
Providing Much-Needed Treatment, Validation and Answers
While the disease is incurable, Dr. Luciano leads a team of fellowship-trained, multidisciplinary colorectal and thoracic surgeons who can diagnose and treat endometriosis even when it has spread onto other organs. Her team at UConn Health also trains fellows to understand, recognize and treat endometriosis while giving lectures and teaching community physicians and providers to increase awareness of the disease.
Increasing awareness is critical as many misconceptions about endometriosis persist, and that can negatively affect diagnoses. “People think they can’t get it because they’re too young when that’s not true. Or they believe it only causes infertility, so it doesn’t matter to them if they have never tried getting pregnant or even plan to do so,” said Dr. Luciano. “These misconceptions can prevent patients from receiving quicker diagnoses until the symptoms become too severe or when they try and can’t get pregnant.”
Another problem lies in what Dr. Luciano referred to as overlapping symptoms. “Endometriosis can cause symptoms that affect the bowel or bladder, so patients end up seeing a gastroenterologist, urologist or physical therapist when they need to visit a gynecologist.”
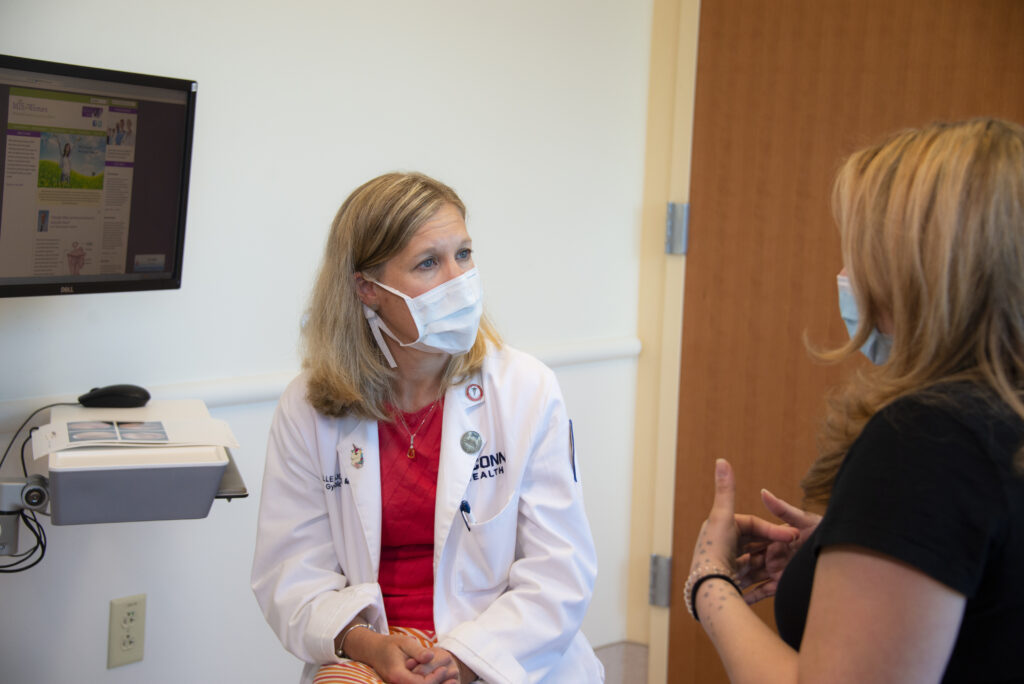
Even physicians’ lack of understanding can cause complications. “Most of the time, the biggest thing my patients are looking for is just someone telling them they aren’t crazy,” said Dr. Luciano. “No, you are not supposed to be this miserable during menstruation. No, intercourse is not supposed to be that painful. Yes, there is a reason for your infertility.”
Women with endometriosis need validation because many of them have already gone to other institutions that not only fail to employ minimally invasive surgeons who specialize in endometriosis but also don’t research the disease. As a result, some physicians don’t know what to do or don’t believe their patients. In contrast, UConn Health has surgeons with expertise in minimally invasive procedures, and endometriosis is a research priority.
“The fact that UConn Health both specializes in and researches endometriosis puts us on the frontline of being able to provide better treatments and diagnoses,” said Dr. Luciano. “About two or three of five new patients I see every day have endometriosis and come to me either because other physicians recommended me or my patients heard about the bill that passed, which made them realize that maybe the symptoms they are having aren’t normal.”
Helping a Unique Bill to Support State-Funded Endometriosis Research
That bill—known as HB 6672—led to the approval of the Connecticut state-funded biorepository, which is planned to open at UConn Health in January of next year. Dr. Luciano played a significant role in promoting the bill because of the research she and UConn Health published in partnership with the Jackson Laboratory. The paper caught the right people’s attention, and she soon was asked to join the Endometriosis Working Group to support Connecticut State Representative Jillian Gilchrest (D-West Hartford), who was spearheading the bill. With the Endometriosis Working Group, Dr. Luciano co-authored the proposal that helped the bill become law.
“What’s really exciting about our biorepository is that it is state-funded,” said Dr. Luciano. “All the other biorepositories in the U.S. are privately owned by one or a group of hospital systems. None of them are state-funded. Kudos to the state of Connecticut for funding this.”
Once the repository opens, Dr. Luciano’s role will be able to recruit her patients whose tissue samples will be collected into the system to help research efforts. “We recently requested the World Endometriosis Association allow our biorepository to be part of a greater worldwide repository so that we can share our knowledge with others and, likewise, gain knowledge from other places around the world and hopefully receive even more diverse samples,” she said. The diversity of samples is critical in understanding and hopefully curing the disease. “Endometriosis affects 10 percent of people born with a uterus, and it doesn’t have any racial propensity, which makes it even more complicated. Being part of a more diverse group of researchers and having access to more diverse tissue samples will help us research. It definitely feels like a dream.”








More Stories
Jamie Shawver, D.O.: The Modern-Day Family Doctor
UConn Health Achieves Excellence in Eye Care in Record Time: Edmund P. Farris, M.D. Chief, Division of Ophthalmology
Leading in Urologic Oncology: Ryan Dorin, M.D., Works on Expanding Patient Care