Photography courtesy of UConn Health
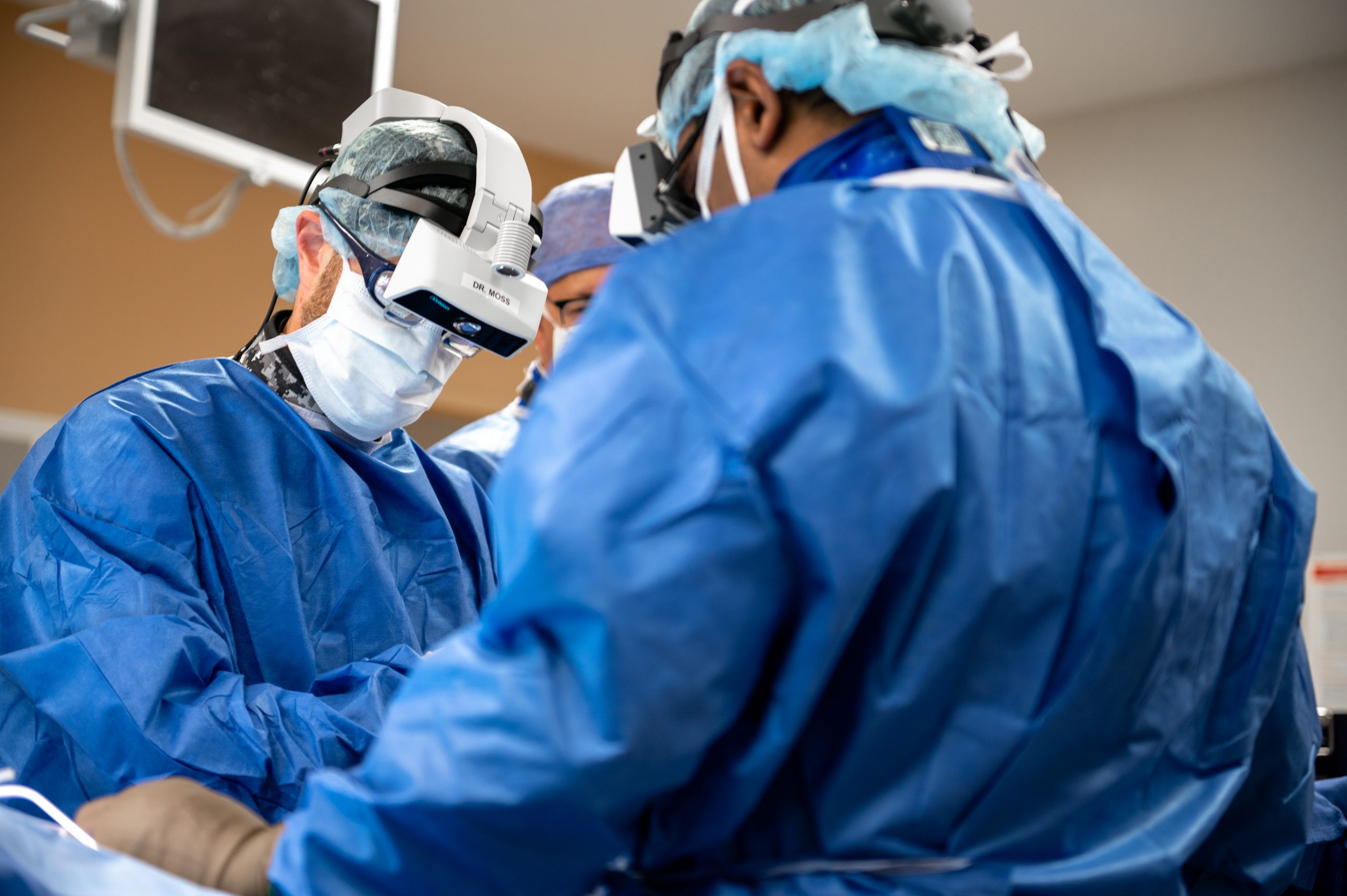
Spine surgeons at UConn Health are using a new technology that enables them to see a 3D image of a patient’s anatomy during surgery. Called augmented reality spine surgery, UConn Health is the first hospital in central Connecticut that has this capability, and has more surgeons trained in the Augmedics’ xVision technology than any other U.S. hospital.
Dr. Isaac Moss, the chair of UConn Health’s Department of Orthopaedic Surgery and co-director of its Comprehensive Spine Center, marveled at how the augmented reality surgical navigation system enables the surgeon to practically see through the patient’s skin.
“I’m a big Superman fan—so this is the closest I think I’ve gotten to X-ray vision,” Moss said. “In fact, the technology is called xVision; the idea is now I’m looking at the patient naturally, but also getting extra information. Navigation is not a new thing, but in traditional navigation systems, the imaging is projected onto a screen. So you’re looking up at a screen while you’re operating instead of the person on the table. This is not a natural way to operate, and there’s a significant disadvantage as your attention is now split between the person that you’re taking care of and the screen, which is giving you the information. With augmented reality technology, all information available is actually projected onto my patient so I can keep my attention focused on exactly what I’m doing at all time.”
Back in May, Moss performed central Connecticut’s first augmented reality spine surgery using the Augmedics xVision and the Airo TruCT Mobile Imaging systems. The operation was a posterior cervical decompression and fusion to address spinal cord compression and progressive weakness, with the new system helping to guide the placement of screws to stabilize the patient’s spine.
Before the arrival of this enhanced spinal navigation system, surgeons would use interoperative X-rays to project a two-dimensional image of the surgical field on a screen. Now, they can work with a 3D field of vision.
With augmented reality, the surgeon dons a wireless headset with glasses inside it and lights and cameras on the outside. The images of the spine are projected onto their retina, enabling them to maintain their focus on the surgical field and not turn their head and look at a screen.
This technology can be utilized in various types of spine surgery from spinal fusion in which screws are inserted into the vertebral bodies to scoliosis correction to treating tumors of the spine and more, said Dr. Hardeep Singh, a spine surgeon at UConn Health. It can be used for minimally invasive procedures or open surgeries.
In the past, surgeons would rely on live X-rays in the operating room and compare them to pre-operative scans or MRIs to guide the surgery.
“With this new technology, there’s less radiation for the surgeon, the room staff and the patient,” Singh said.
Dr. Ian T. McNeill, a UConn Health neurosurgeon and co-director of scoliosis and spinal deformity surgery, likened the augmented reality technology to using a GPS while driving.
“If I’m driving to West Hartford, I know the way, but I still use the GPS to find the best route and timing,” he explained. “Similarly, we already know how to place screws, but augmented reality allows us to be as perfect as possible. It’s not required but it gives us enhanced accuracy and precision.”
The spine is “valuable real estate,” and any technology that improves outcomes should be embraced, McNeill added.
For the patient, greater precision means greater accuracy, helping the surgeon to minimize soft tissue damage, instrument the spine with greater speed and lessen the anesthesia time, leading to a faster recovery and decreases in post-operative pain, McNeill said.
While every patient is different, Singh stated that most patients with minimally invasive spine surgery recover faster, have lower blood loss and generally require a shorter hospital stay, while those who have had open procedures tend to require a longer hospital stay.
All the surgeons at the UConn Health Comprehensive Spine Center are fellowship-trained, which means they have completed the most advanced, subspecialized training in their field. Moss completed his fellowship at Rush University Medical Center in Chicago studying advanced spinal and scoliosis surgery. He also has a master’s degree in biomedical engineering.
McNeill is a dual fellowship-trained neurosurgeon. He completed one fellowship in complex spine surgery at the Icahn School of Medicine at Mount Sinai and a second orthopedic spine fellowship in adult and pediatric spinal surgery at the University of California at San Francisco.
Singh completed a spine surgery fellowship at Emory University Orthopaedics and Spine Hospital focused on treating patients with complex spinal pathologies including scoliosis and deformity correction, trauma, tumor and infections of the spine.





More Stories
Driven by Dedication to Excellence in Patient Care
Setting the Standard for Surgical Care at Saint Francis Hospital: How Kelly Tyler, M.D., and a Multidisciplinary Team Are Advancing Surgery in Connecticut
Innovation and Dedication that Prioritizes Patient Care