UConn Health Stroke Program
By Alix Boyle / Photography by Tina Encarnacion
UConn Health recently received certification as an advanced thrombectomy-capable stroke center. It’s the first such program in the greater Hartford area and only the second in Connecticut.
This means that patients will receive the fastest, most comprehensive care possible.
In the case of a stroke, a thrombectomy is a minimally invasive surgery to remove a blood clot from an artery in the brain.
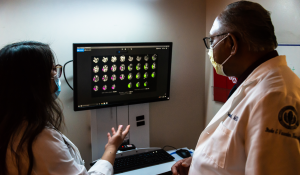
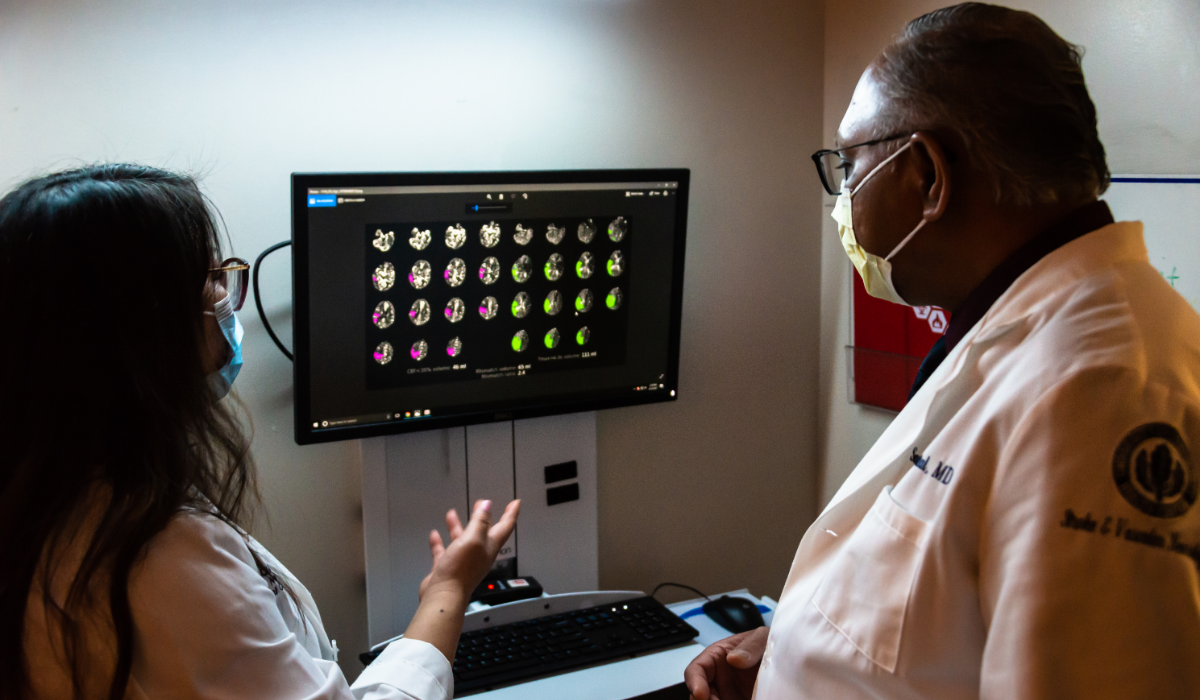
“Our multidisciplinary team includes neurocritical care intensivists, neuro-interventionalists, neurosurgeons, vascular neurologists, and a stroke nurse navigator,” said Dr. Sanjay Mittal, a neurologist and medical director of the stroke center. “This collaboration can really optimize patient outcomes. Additionally, our EMS partners are such a strength of the program.”
There are two types of strokes. Ischemic strokes account for the vast majority and occur when clots block the blood vessels to the brain and cut off blood flow. Hemorrhagic strokes happen when the wall of a blood vessel breaks and blood leaks into the brain.
Not all hospitals are equal when it comes to stroke care. Some hospitals are only capable of stabilizing patients until they can be treated at another hospital that offers appropriate care. Others are considered capable of caring for stroke patients, and a few, like UConn Health, offer the full spectrum of treatments.
“Time is brain,” said Jennifer Sposito, a nurse who is the clinical coordinator of the stroke program. “This special certification that we recently received is great for our population because people need to get quick care near where they live. We want to save whatever brain function we can. Time could mean the difference between a severe disability or a minor one or the ability to walk and talk.”

At UConn Health, stroke care begins when emergency medical services (EMS) arrives for the patient. UConn John Dempsey Hospital receives stroke patients from 15 different towns and ambulance services, so there’s a big emphasis on training first responders about recognizing the signs and symptoms of a stroke.
UConn Health publishes a monthly newsletter for the first responders including information on strokes, and all are required to earn continuing medical education credits.
For example, there’s a reminder that even though patients are not presenting with classic symptoms, they may still have had a stroke. Those include “sudden altered mental status, vision disturbances, and/or altered equilibrium/vertigo,” according to the newsletter.
“We are equal partners in our patients’ care,” said Peter Canning, a paramedic, nurse, and EMS coordinator for UConn Health. “There’s a big emphasis on quality assurance. The sooner the EMS recognizes it’s a stroke, the better the patient’s outcome.”
The ambulance aims to arrive within 8 minutes of the 911 call and spend no more than 15 minutes on scene. Once the paramedic determines the patient may be having a suspected stroke, they call the hospital with a “STROKE ALERT” so that when the patient arrives, they can be brought directly to CT scan on the EMS stretcher. “The team is standing by to swarm the patient,” Canning said.
If the CT scan shows evidence of a clot, the patient may be prescribed the clot-busting drug tPA (tissue plasminogen activator). This must be administered within three to four and a half hours of the onset of the stroke.
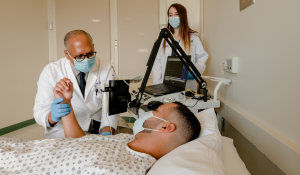
Or, depending on where in the brain the stroke is located, the patient may be a candidate for a thrombectomy. “Our teams decide which treatment to use following the latest literature, research, and guidelines outlined by experts in the field and also as recommended by the American Heart/American Stroke Association,” Sposito said.
UConn Health offers a free stroke education symposium every year for first responders and health care providers. During COVID-19, the event was held virtually.
As the population ages, stroke is only going to become more common, and it’s important for all of us to learn the signs and symptoms, Canning said.
Sposito recommends learning the BE FAST acronym. Call 911 if you suspect someone is having a stroke.
Balance – Watch for a sudden loss of balance.
Eyes – Check for vision loss.
Face – Look for an uneven smile.
Arm – Check if one arm is weak.
Speech – Listen for slurred speech.
Time – Call 911. Time is of the essence in treating stroke.
There are also numerous medical conditions and lifestyle choices that are personal risk factors for stroke. These include atrial fibrillation, high blood pressure, high cholesterol, heart disease, prior stroke, alcohol use, smoking, obesity, and physical inactivity.
“Back in 2013 we realized our community needed stroke care,” Sposito said. “The first stroke alert was in 2014.” A stroke alert is a standardized protocol for how a hospital treats stroke patients.
“Ever since then, we have been growing the program and striving for excellence. We’ve had many additions to our team including a neurocritical care intensivist. We continued to grow, added a neurosurgeon and a neuroradiologist, and in 2017, we did the first thrombectomy. Now there are two providers who can perform endovascular thrombectomy.”
Since 2017, UConn Health has performed more than 100 thrombectomies and currently does two or three a month.
Mittal, the director of the program, cares for hospitalized stroke patients. Additionally, he works on stroke prevention and manages patients with post-stroke muscle spasticity.
This certification from the Joint Commission is important because it lets patients know that the UConn Health stroke program has reached the highest level of quality and safety. UConn John Dempsey Hospital has also earned the “Gold Plus” designation for the past six years from the American Heart Association’s “Get With the Guidelines” program for top-quality stroke care.
“There are a select few programs who demonstrate top care,” Sposito said. “It speaks very highly of our staff and for our global drive of patient safety and quality improvement.”






More Stories
UConn Health Achieves Excellence in Eye Care in Record Time: Edmund P. Farris, M.D. Chief, Division of Ophthalmology
Specialty Care for Melanoma at UConn Health
Danielle E. Luciano, M.D.: Increasing Awareness and Treatment for Endometriosis